By: Patsy Catsos, MS, RDN, LD, Private Practice Dietician and Co-Author of IBS-Free Recipes for the Whole Family
People with functional gut symptoms have known for years that food choices can impact symptoms. Yet, common diet advice (such as to eliminate red meat and spicy foods and add high-fiber foods and increase fluids) often fails to deliver relief.
Cathy F., a 55-year old client of mine, had constipation predominant irritable bowel syndrome (IBS-C) for years. As a result, she suffered from hemorrhoids, anal fissures, and a rectocele, for which she’d had several surgeries.
Her well-meaning healthcare providers recommended a high-fiber diet.
Cathy did her best for many years to follow this advice, and her regular diet included bran cereal for breakfast every day, apples for soluble fiber, fiber-fortified breads and bars, and large portions of nuts. She kept a food and symptom diary for years, yet was unable to spot individual food triggers.
What’s a FODMAP?
FODMAP is the acronym for a group of osmotically active, rapidly fermentable, short-chain carbohydrates. It stands for Fermentable Oligo- Di- and Monosaccharides and Polyols.
Examples of FODMAPs are lactose, fructose, sorbitol, mannitol, fructooligosaccharides, and galactooligosaccharides. The concept originated with scientists at Australia’s Monash University.
I suggested Cathy try a short dietary experiment: a FODMAP elimination diet.
This is a new evidence-based approach to helping people with IBS identify which foods are well-tolerated and which foods are not.
The FODMAP elimination diet is a process, not a list of acceptable foods.
Cathy began by eliminating high FODMAP foods from her diet for a few weeks.
Then she followed a detailed plan that we created together to reintroduce each type of FODMAP back into her diet one at a time, monitored her symptoms, and adjusted her diet accordingly.
FODMAPs are an irresistible topic for bloggers, social media, and mainstream print media, with some of the best hooks an editor could want: What Your Doctor Never Told You, An Apple a Day – Not, Australian Researchers Discover New Diet Secret, and so on.
Unlike many other diets making headlines, the low-FODMAP diet does have a developing body of solid research to back it up. Studies have shown it can help up to 85% of well-selected patients with IBS achieve relief of their symptoms. But, it isn’t right for everyone.
Have you been thinking about trying a low FODMAP diet, or have you already started?
If you do decide to try it, be sure to avoid these common low FODMAP diet pitfalls:
Starting the Diet Without Medical Advice
Don’t diagnose yourself with IBS. Start with your primary care provider (PCP) to discuss your symptoms, diagnosis, and treatment. If necessary, your PCP will refer you to a gastroenterologist.
Once you have a confirmed diagnosis of IBS, seek out a registered dietician with FODMAP experience, if available. Most physicians don’t have the time or skills to perform a thorough nutrition assessment.
In my practice I find some people are not good candidates for an elimination diet, particularly those at risk for eating disorders, those with little control over their food (such as people living in community situations), and those whose diet history reveals that they are already following an instinctively-determined low FODMAP diet.
If there are many foods you can’t eat due to other medical conditions, inflexible food preferences, or your food philosophy, you will need extra help meeting your nutrient needs on a low FODMAP diet.
Expecting Too Much
It’s important to have realistic expectations about what FODMAPs can do for you. Learning more about how your body reacts to FODMAPs can empower you to manage your IBS more effectively.
How important is that? Ask Cathy, who revealed at our second visit, “Until now, I never knew what it felt like to be normal.”
However, since FODMAPs themselves are not the root cause of IBS, eliminating them won’t cure the condition. Though most people eventually return to a modified version of their preferred diet, there will probably be some foods you must learn not to overdo.
Changing Everything at Once
If you are changing your diet, medications, and supplements all at the same time, how will you know what worked? You will learn more from the elimination and reintroduction process if you keep the rest of your regimen stable for a few weeks while you experiment.
Work with your other healthcare providers to negotiate this, perhaps delaying proposed new prescription medications or supplements until after the first few weeks on the diet.
If you are to be treated with antibiotics for small intestinal bacterial overgrowth (SIBO), it is often best done immediately before beginning a low FODMAP diet.
Over-Limiting Your Diet
Be sure to eat a wide variety of low FODMAP foods unless you have an important reason not to. For example, lactose is the only component of dairy products that must be avoided on a low FODMAP diet.
Unless you are a vegan or are allergic to milk, you can continue to use low-lactose milk products such as aged cheeses and lactose-free yogurt on the diet.
Likewise, oligosaccharides (certain fibers) are the component of soy or wheat that should be avoided on a low FODMAP diet.
Processing methods that reduce oligosaccharides can make certain wheat or soy foods suitable for the diet. Authentically made sourdough bread and tofu, for example, are low FODMAP foods.
Inadequate Fiber Intake
Fiber intake can take a hit on a low FODMAP diet. That’s not ideal, since fiber is an important food source for the good bacteria in our gut. In addition to producing gas, those gut bacteria perform other services important to human health.
The solution is to deliberately increase your intake of fiber from low-FODMAP foods: eat a wide variety of low FODMAP fruits and vegetables, grains and legumes, and small servings of nuts and seeds.
Low FODMAP fibers are fermented more slowly and are less likely to disrupt fluid balance in the gut. See the Table accompanying this article for specific suggestions.
Conclusion
The last time I saw Cathy her symptoms were well controlled on a moderately low FODMAP diet. During the reintroduction process she discovered that lactose and oligosaccharides were significant symptom triggers for her, so she consumes low-lactose milk products only; sticks to small portions of foods like wheat, beans, and nuts; and gets more fiber from foods like quinoa and chia seeds. With choices like these, Cathy is avoiding the common pitfalls and eating the most varied and nutrient-rich diet she can tolerate.
Table
Sample of Low FODMAP Foods Adapted from IBS-Free Recipes for the Whole Family by Patsy Catsos, Lisa Rothstein, and Karen Warman and used by permission. 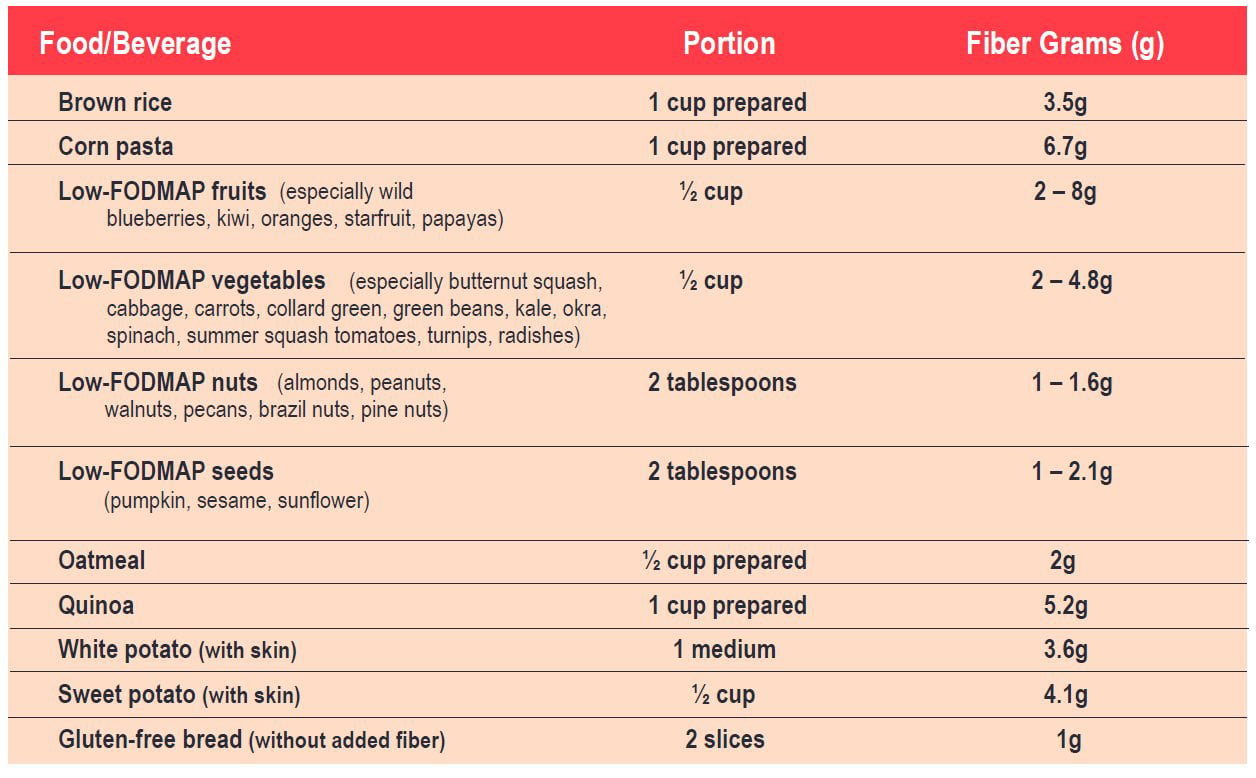
The Table above provides examples, not meant to be a complete list. Why do various lists sometimes differ? Find the answer here.
Adapted from IBS Publication
Adapted from IBS Publication #271- Five Low FODMAP Diet Pitfalls (and What You Can Do to Avoid Them) by Patsy Catsos, M.S., R.D.N., L.D., Private Practice Dietician and Co-Author of IBS-Free Recipes for the Whole Family
