The first step in making diagnosing IBS is for the healthcare provider to identify if an individual has symptoms of IBS.
Originally, the diagnosis of irritable bowel syndrome (IBS) was thought to be a “diagnosis of exclusion”. This implies that the diagnosis of IBS was valid only if other disorders that may be causing symptoms were ruled out. Today, healthcare providers agree that tests may be necessary to rule out other diagnoses. However, these tests should only be limited to those necessary, based on symptoms and medical history. IBS is a specific condition that can be confidently diagnosed based on a good understanding of the symptoms experienced, following a comprehensive history and physical examination and in the absence of alarm signs.
What is IBS?
Irritable bowel syndrome (IBS) is a disorder characterized by two key elements:
- an abdominal component generally described as pain and/or discomfort and
- a change in bowel habits which could include:
- changes in stool texture – how the bowel movement (BM) looks and/or
- Frequency- how often you have a BM
A change in bowel habits can be any change from what is normal for you, such as how often you have a bowel movement or what the BM looks like (how watery or solid, its color, how much you expel at a time). Changes in stool texture includes experiencing constipation, diarrhea, or both.
- Constipation is commonly defined as having three (3) or fewer bowel movements (BMs) a week, and/or difficulty passing BMs.
- Diarrhea is defined as loose, watery, or frequent BMs.
Diagnosing IBS
IBS can be confidently diagnosed based on a good understanding of the symptoms experienced, following a comprehensive history and physical examination and in the absence of alarm signs. Minimal testing may be required to rule-out other disorders as potential causes of symptoms.
In the 1990’s, a group of healthcare providers created the first standard for evaluating irritable bowel syndrome (IBS). Called the Rome Criteria, this criterion is considered the “gold standard” for the diagnosis of IBS for clinical research studies.
The Rome IV diagnostic criteria for IBS states that those with IBS have certain symptoms that must have been present for the past three (3) months and started at least six (6) months before. They will have abdominal pain at least one day each week, along with at least two of the following:
- The abdominal pain is associated with a bowel movement, or
- a change in how their bowel movements look, or
- a change in how often they have bowel movements.
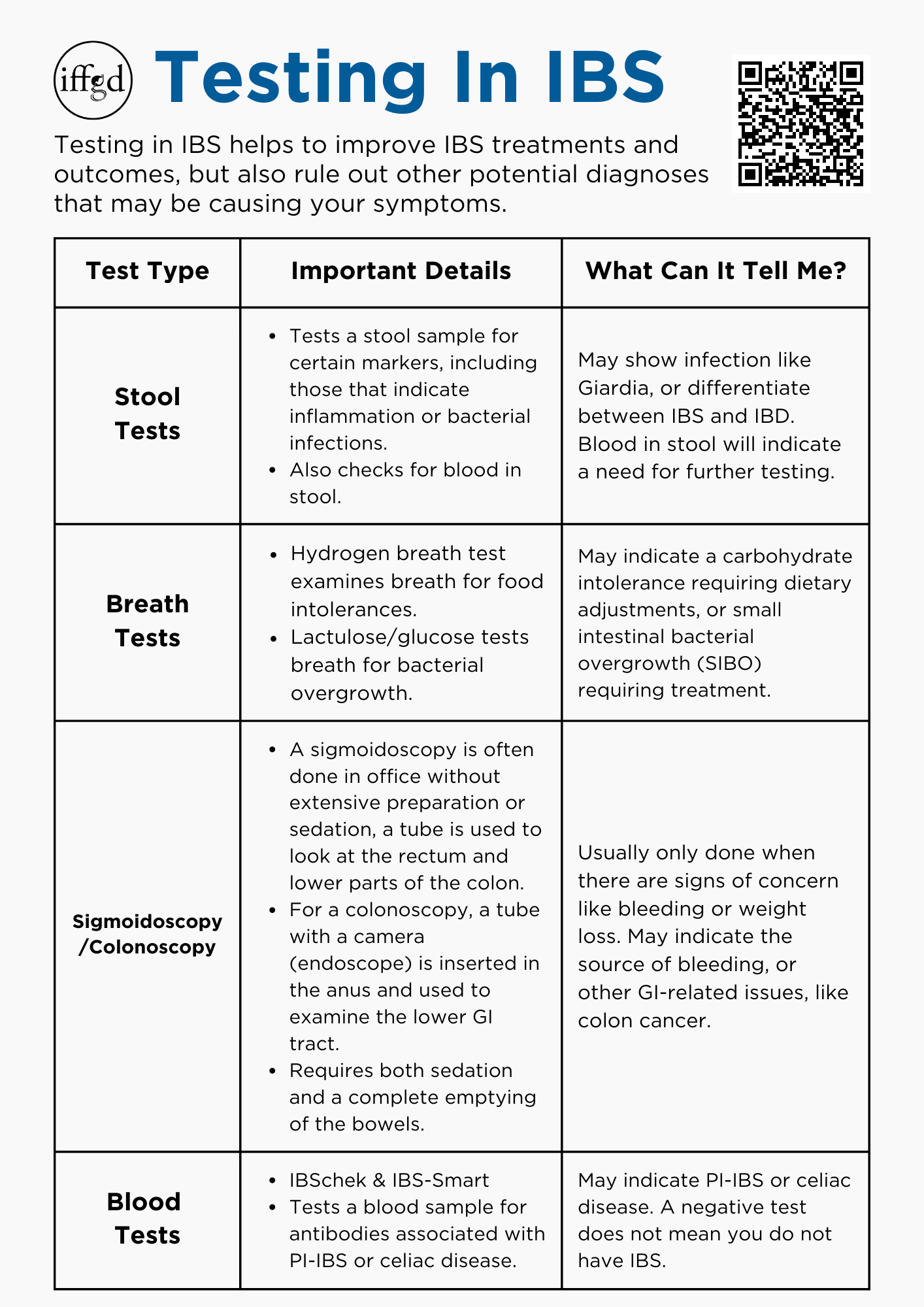
Blood Tests
There are two blood tests designed to assist with the diagnosis of IBS. They are IBSchek and IBS-Smart. Both are blood tests designed to assist in the diagnosis of irritable bowel syndrome with predominant diarrhea (IBS-D) or with mixed bowel habits (IBS-M) in adults. They do this by testing for certain antibodies thought to be related to IBS developed after a GI infection (post-infectious IBS).
Some research studies have shown that patients with IBS-D or IBS-M have high positivity rates of these antibodies when compared with healthy patients. However, these antibodies do not detect IBS in everyone, and a negative test does not mean you do not have IBS.
A blood test may also be used to screen for celiac disease.
- Celiac disease is a genetic condition of the small intestine that develops in people who are unable to eat gluten (a common ingredient in many foods including grains, wheat, rye, and barley, as well as many processed foods). It causes malabsorption of nutrients and food and results in symptoms similar to those in IBS.
Generally, screening for celiac disease with blood tests is recommended in those with irritable bowel syndrome with diarrhea (IBS-D). If the blood test is positive, an upper endoscopy should be performed to examine and biopsy the small intestine to confirm the diagnosis. The healthcare provider may also check for inflammatory bowel disease (IBD) by testing to see if certain proteins are present.
Stool Tests
The most common reasons to test a sample of a bowel movement is to check for
- bacterial infections (specifically Giardia- a tiny parasitic germ that causes giardadsis (a disease-causing diarrhea). Giardia can be found on surfaces, in soil, food, or water contaminated with feces (poop) from infected people or animals. This infection should be only considered in patients with exposure or risk factors.),
- inflammation (testing for fecal calprotectin and lactoferrin is used to see if there is inflammation in the gastrointestinal tract. This helps to determine if someone has inflammatory bowel disease (IBD) and/or irritable bowel syndrome (IBS).
- blood in the BM (a positive fecal blood test indicates that there is bleeding somewhere in the digestive system and will require further testing to determine where it is coming from).
Learn more about testing in IBS.
Summary
IBS can be confidently diagnosed by a careful review of symptoms, a physical examination, and minimal diagnostic testing. Individuals with IBS-D should be tested for celiac and IBD. Those with IBS-C require no diagnostic testing and evidence-based treatment is recommended for initial treatment of symptoms. If these treatments fail; however, anorectal manometry and balloon expulsion testing should be performed to rule-out issues with the pelvic floor. With an accurate diagnosis, both patient and provider can work together on the most effective management.
Adapted from IFFGD Publication #163: Current Approach to the Diagnosis of Irritable Bowel Syndrome By: Leila Neshatian, MD, MSc, Clinical Associate Professor, Stanford University School of Medicine and Sarvee Moosavi, MD, FRCPC, Clinical Assistant Professor Neurogastroenterology and GI Motility, University of British Columbia, Vancouver General Hospital, St. Paul’s Hospital GI Motility Lab Edited by: Darren M. Brenner, MD, Professor of Medicine and Surgery, Northwestern University – Feinberg School of Medicine, Chicago, Illinois
